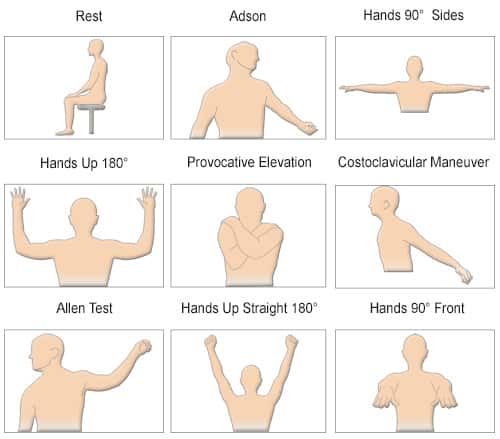
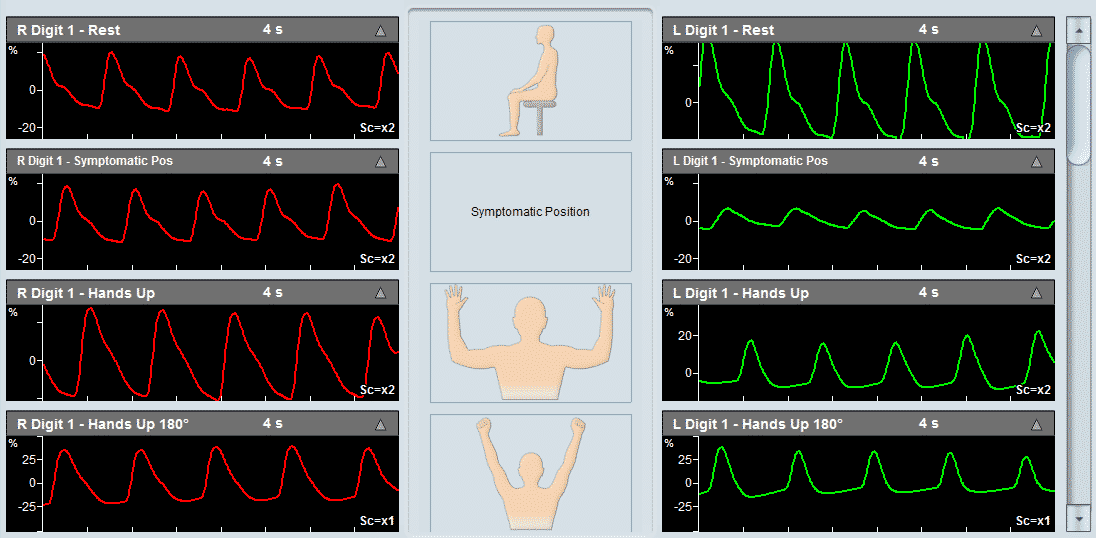
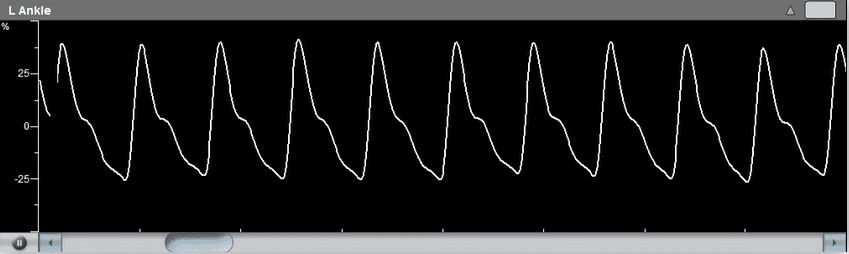
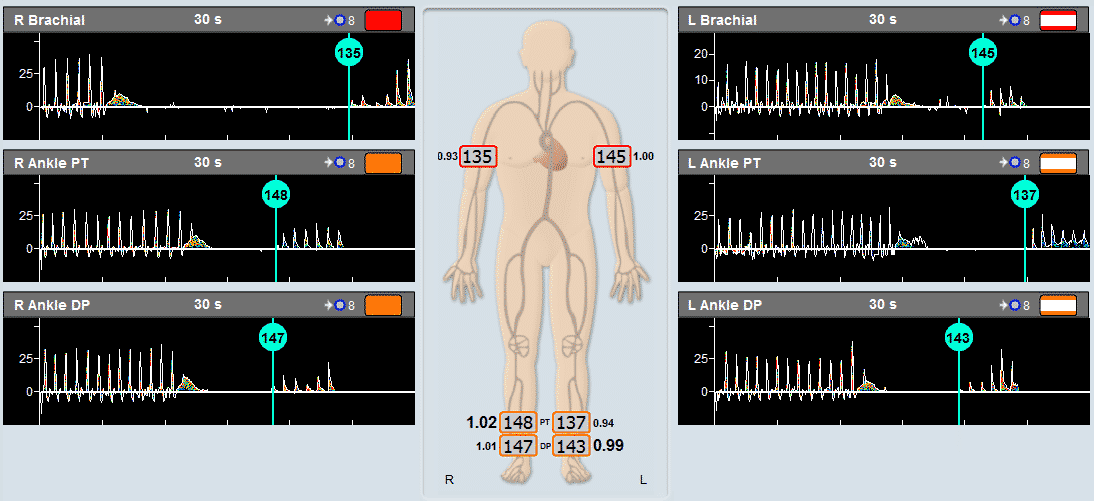
Detection and monitoring of vasospasm – one of TCD’s strongest points
The scan can be performed daily, at the bedside, in ICU, and involves no exposure to radiation, magnetic fields or contrast dyes. It is a far cheaper and easier logistically than CT, MRI or angiography and there are no issues with radiation, repeat testing on patients with reduced renal function.
Diagnosis of intracranial artery stenosis in the setting of stroke, and confirmation of the severity and significance of artery stenosis in the neck. This examination may assist in surgical planning and risk determination.
Can detect emboli due to significant artery stenosis, which is an indicator of increased stroke risk, and assist in the management of patients with non-symptomatic carotid artery disease.
Monitoring of cerebral vascular autoregulation during anaesthesia; assisting in managing patient vital parameters in order to reduce the risk of cerebral oedema and hyperperfusion injury during surgery.
Detection of right-to-left heart shunt and PFO (patent foramen ovale)
The TCD can detect significant cardiac defects that lead to an increased risk of stroke or TIA, all done in a cost effective and minimally invasive examination compared with other techniques – only an intravenous cannula is needed, no anaesthetics, sedation or contrast dyes required
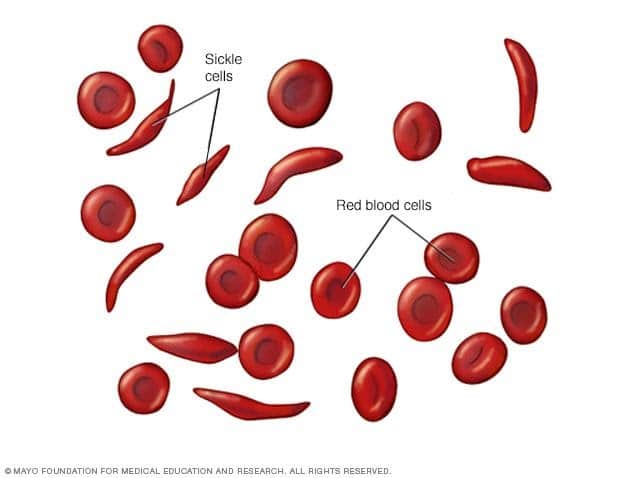
Treatment planning and monitoring of patients with sickle cell anaemia; After diagnosis, TCD can detect the arterial stenosis associated with sickle cell anaemia, and guide clinical decision making regarding the need for treatment via blood transfusions in order to reduce the risk of stroke.
Intra-operative detection of emboli
TCD can be used to detect emboli occurring both during vascular surgery and postoperatively, and give an indication of patients who are at increased risk of stroke; and
TCD can be used to optimise post-operative monitoring and anticoagulant treatment for those patients at greater risk of stroke and other vascular events.
TCD can also be used to help in confirming brain death, in association with a variety of other clinical markers.
Arteriovenous Malformation
AVM relates to a condition whereby the arterial flow bypasses the capillary circulation and connects directly to the venous drainage, thus not allowing for appropriate tissue perfusion.
This condition is characterized by low resistance, hence high-volume flow rates. TCD will detect high mean velocities – although lower then with severe vasospasm – coupled with low pulsatility indices.
Brain Death
This condition reflects an extensive and irreversible brain damage, characterized by almost no volume blood flow to the brain.
TCD can detect the different brain death stages through analysis of the particular waveforms: a sharp systolic peak followed by near zero diastolic velocities; systolic spikes followed by retrograde diastolic velocities; short spikes; and ultimately, no signals at all.
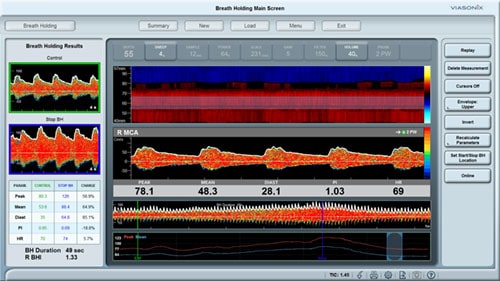
Cerebral Vasomotor Reactivity and Autoregulation
CVR and autoregulation define the physiological compensatory mechanisms when flow is impaired. Identification of exhausted CVR can be a good indication for high risk for stroke.
CVR can be assessed with TCD under two monitoring conditions: hypercapnia or CO2 reactivity, and with intravenous injections ofAcetazolamide or the Diamox test.
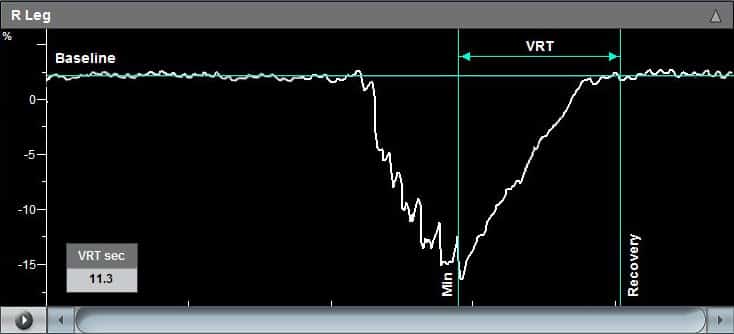
Typically, an increase in peak velocities above 40% after the perturbation reflects intact CVR, whereas smaller increase reflect different degrees of impaired CVR. Absence of flow increase reflects a complete exhaustion of the autoregulatory capacity.
Collateral Capacity
Similar to CVR, collateral flow reflects an alternative compensatory mechanism to pathological flow conditions. The cerebral collateral pathways include side-to-side via the anterior communicating artery, posterior-to anterior via the posterior communicating artery, and external-to-internal via the ophthalmic artery.
TCD will detect reverse velocities in the collaterally perfused arteries, indicating the viability or absence of this compensatory mechanism.
Emboli Detection
Cerebral emboli can take the form of atherosclerotic plaques, air bubbles or blood clots. The immediate risk of cerebral embolization is in impaired perfusion which may lead to stroke and death.
TCD can detect the embolic signals in the blood flow velocity waveforms, which are characterized by high intensity, short duration and unidirectional signals.
Evaluation of ICP Changes
Elevated ICP will result in a decrease in the cerebral perfusion pressure, and ultimately in cerebral perfusion. Therefore, controlling ICP from increasing too much is critical to prevent brain ischemia.
With TCD, qualitative assessment of ICP changes can be made. Since elevated ICP increases significantly the distal resistance, typically the effect on the TCD signals will be reduced velocities, coupled with a sharp increase in the pulsatility indices.
ICU or Monitoring (OR Monitoring)
This setting for cerebral monitoring is critical for identification of neurologic complications.
Relative and/or sudden changes in the cerebral blood flow velocities can become a powerful diagnostic tool and effect the immediate clinical intervention.
Intracranial Stenosis
This condition relates to a focal narrowing of the artery, either as a result of an atherosclerotic lesion or as a result of external compression due to a tumor.
TCD will easily identify a local increase in blood flow velocities, characterized by the fact the at a greater or smaller depth the velocities will be much lower.
Peak focal velocities above 150 cm/sec reflect arterial stenosis. However, if the severity of the stenosis is beyond its’ critical level, velocity signals may be diminished.
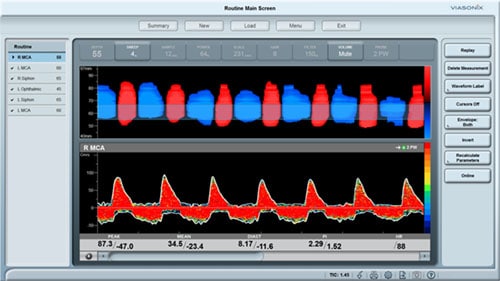
Vasospasm and SAH
Cerebral vasospasm is typically the outcome of SAH as a result of an aneurysm rupture. Early detection of vasospasm is critical since it allows timely intervention.
TCD is rather specific for this condition, and allows non-invasive, continuous bed-side monitoring.
Vasospasm is characterized by increased velocities due to arterial narrowing. Severe vasospasm is when mean velocities exceed 200 cm/sec, moderate conditions are with mean velocities between 120-200 cm/sec, and moderate vasospasm is for mean velocities near 120 cm/sec. Additionally, velocities in the middle cerebral artery can be compared to internal carotid artery velocities, and the resulting ratio (Lindergaard index) can indicate cerebral vasospasm when it is greater than 3.