What is Raynaud’s Syndrome?
Raynaud’s Disease is a disorder of the blood vessels, in which spasm of the blood vessels causes them to narrow under certain conditions, typically triggered when exposed to low temperatures or feeling stressed. This narrowing, in turn, results in reduced blood perfusion to the affected sites, most frequently the peripheral vessels in the fingers or toes.
This disease is often called also Raynaud’s Syndrome or Primary Raynaud’s. When also accompanied by an arterial obstruction, it is referred to as the Raynaud’s Phenomenon or Secondary Raynaud’s. When Raynaud’s occurs, blood cannot reach the surface of the skin, and the affected areas can turn white or blue. In severe cases, loss of blood perfusion can cause sores or even tissue death.
The prevalence of Raynaud’s Syndrome is in roughly 5% of the population, with a significantly higher occurrence of Raynaud’s in females.
It is also more frequent in regions with cold climate. Smoking and alcohol consumption are among the risk factors for this disease.
How to Test for Raynaud’s Disease
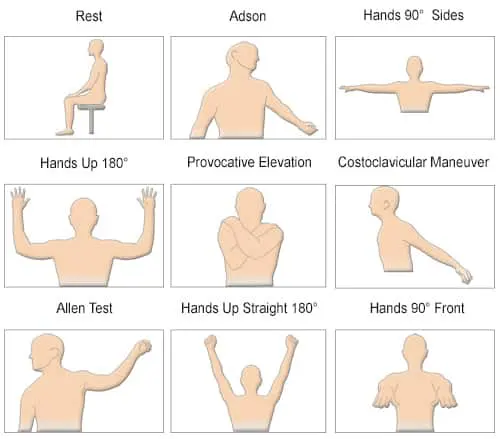
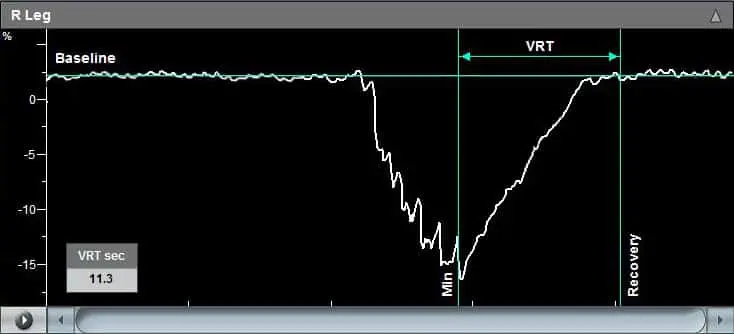
The physiological diagnosis of Raynaud’s Disease is typically performed by measuring the PPG (photoplethysmography) waveforms and/or the digit/toe blood pressures at room temperature and after cold immersion. The response of the measurements to the exposure to cold water immersion and the recovery time post cold immersion are essential in diagnosing the disease.

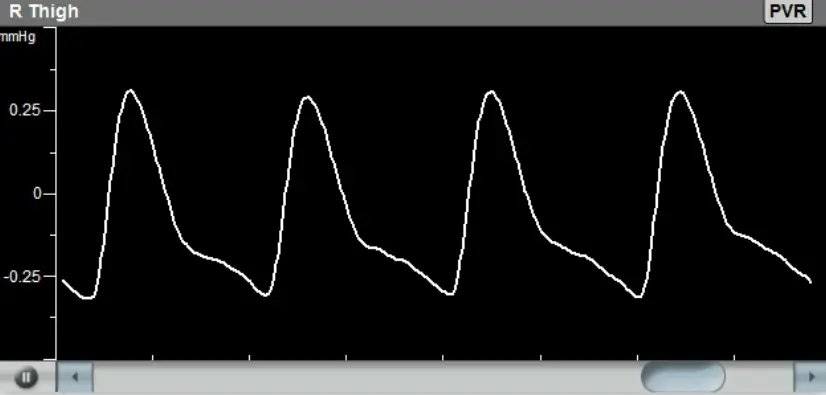
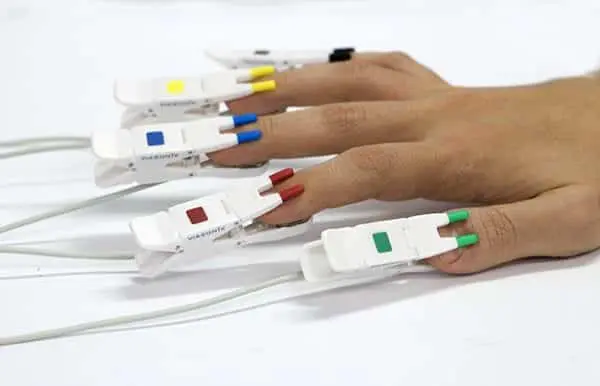
PPG Sensors
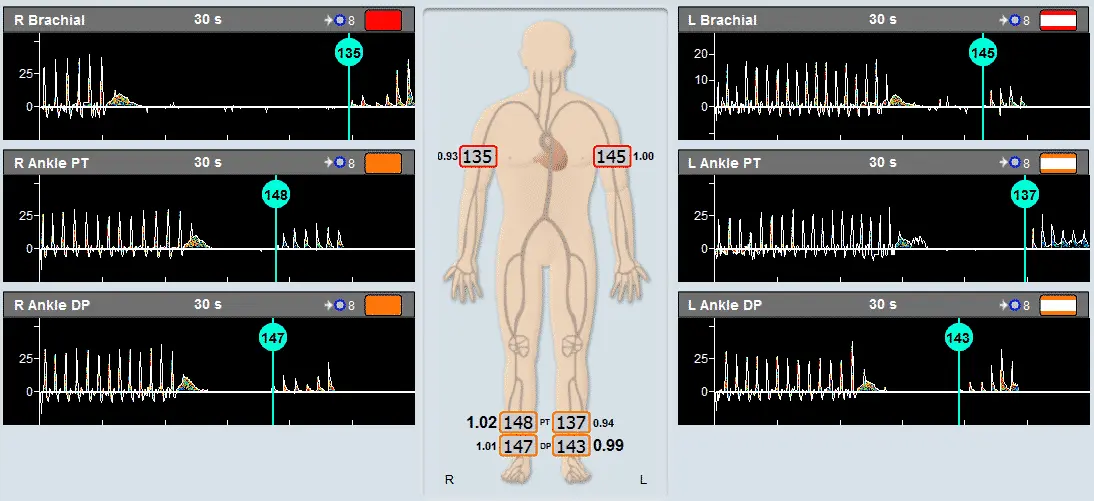
Secondary Method of ABI Assessment

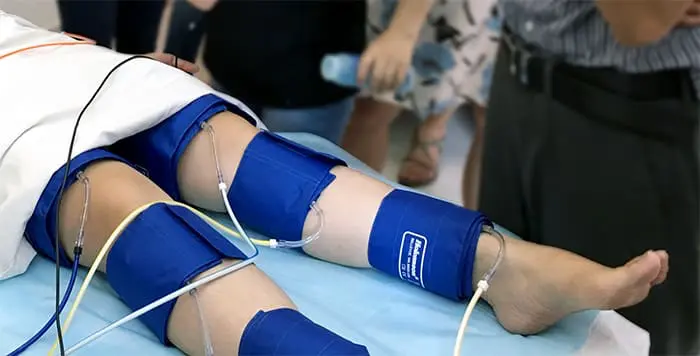
Inflatable Cuffs
High quality available in a variety of sizes
Using the Falcon for Raynaud’s Measurements
The Falcon/PRO system has a dedicated Raynaud’s test protocols:
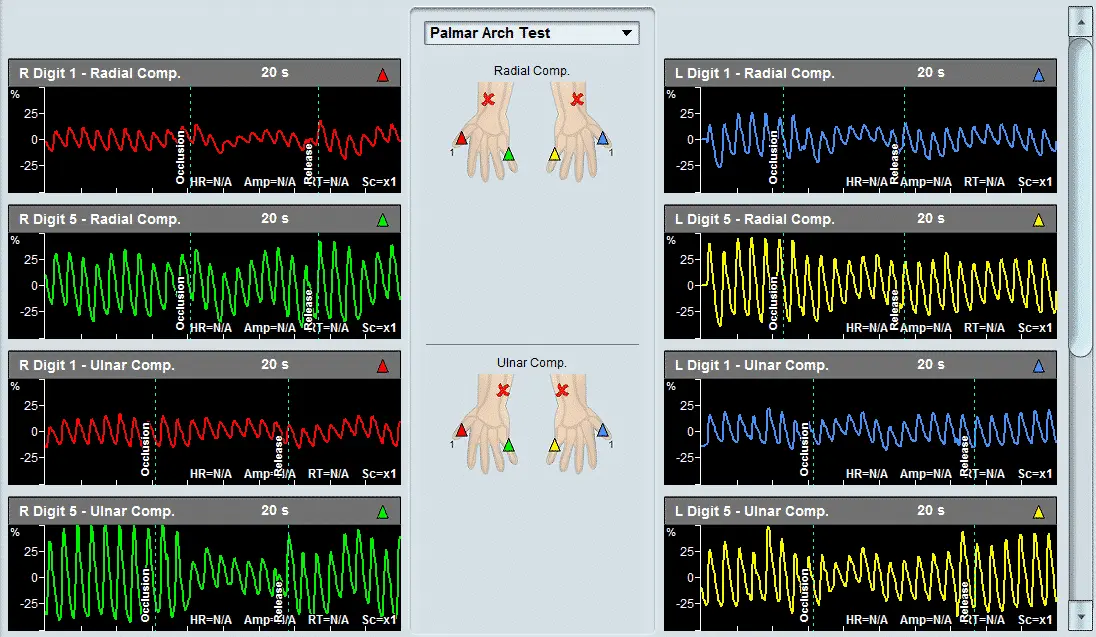
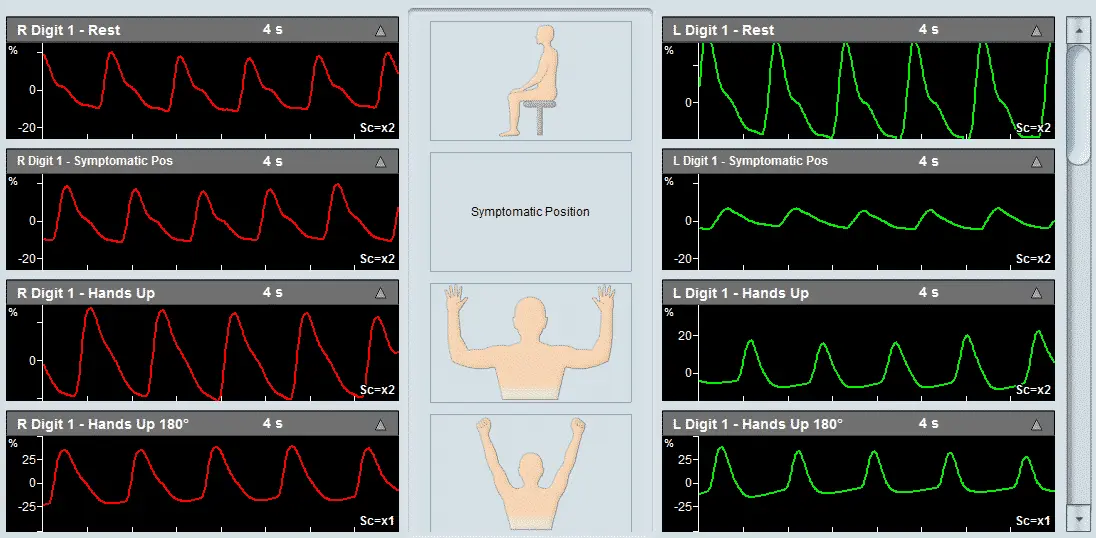
- Measuring the PPG waveforms on all 5 fingers or toes,
- A protocol for simultaneously measuring the systolic blood pressure at each of those sites.
These protocols are supported by the 5 color-coded PPG sensors and 10 independent pressure channels of the Falcon system. This design allows for rapid and simultaneous measurement of the PPG waveforms and/or the systolic blood pressure in all 5 fingers or toes at the same time and in a single test. This type of examination is crucial when performing Raynaud’s diagnosis because the patient needs to immerse the hand (or foot) in cold water only once and does not need to repeat the cumbersome (and sometimes painful) process separately for each finger or toe.
The Falcon also has an integrated temperature sensor, which is important in documenting the skin temperature during the cold immersion, and then continuously monitoring the skin temperature during the recovery period. The time display of the measurements can be changed from 1 second and up to several minutes, which allows focusing on a specific phenomenon or view the signal trends.
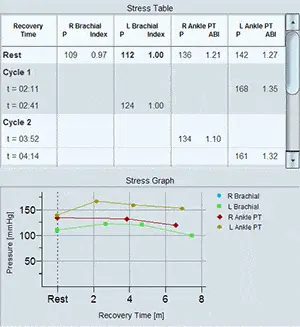
Various print and report options are specifically designed for a detailed comparison between the pre- and post-immersion results. The PPG waveform amplitude and systolic rise time parameters are presented for PPG analysis, and the systolic blood pressure differences are presented in a graphical manner to highlight possible pathology.
Expected Results
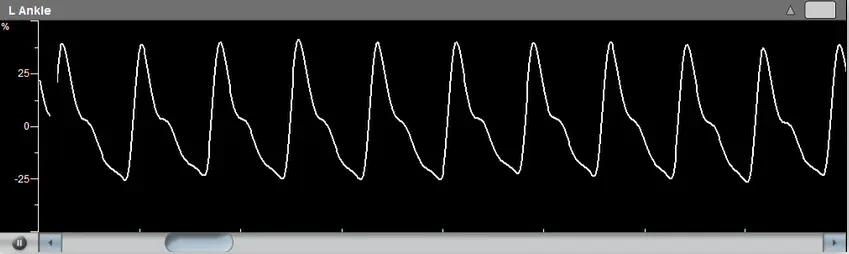
When measuring only the PPG waveforms, the focus is on the time of return of the PPG waveforms after cold immersion to the amplitude levels that were measured pre-immersion.
A return of the waveforms within 10 minutes or so to the levels prior to the cold immersion challenge is sometimes considered normal, while a longer duration may indicate a disease condition.
Pressure measurements are sometimes used to discriminate between Raynaud’s secondary to arterial obstructions. A decrease in systolic blood pressure is typically observed in secondary Raynaud’s patients compared to those with primary Raynaud’s.