Posts
- Interesting Questions from A Vascular Ultrasound Laboratory
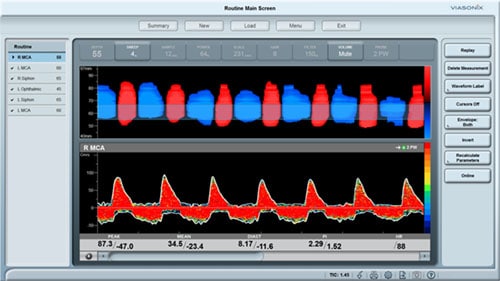
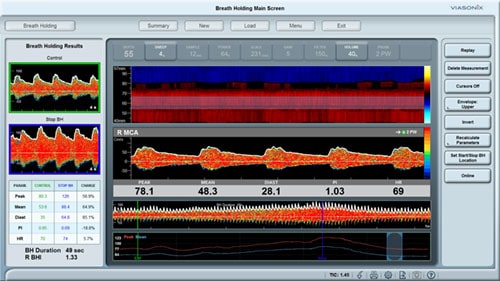
- Feedback from a neurology surgeon at a hospital after using Transcranial Doppler (TCD) to track vasospasm
- The clinical benefits, applications and usage of Photoplethysmography (PPG) sensors in a vascular laboratory
- How To Select The Right Transcranial Doppler Equipment For Your Clinic?
- Exploring and comparing the Various Transcranial Doppler Applications in Neurology and Stroke Management
- 5 Reasons to use Transcranial Doppler Instead of an MRI
- What Are The Latest Advances in Transcranial Doppler Technology for Non-Invasive Monitoring of Cerebral Blood Flow
- Technical Benefits and Features of the Dolphin IQ & 4D
- Clinical Applications of Transcranial Doppler (TCD)
- What Is Transcranial Doppler?
- Spider and Varicose Veins
- Peripheral Artery Disease and It’s Treatment
- Peripheral Vascular Disease – Facts and Information
- Non-Invasive Examination for Vascular Diseases
- An Overview on Peripheral Vascular Diseases
- A Short Guide About Peripheral Vascular Diseases
- Raynaud’s Syndrome: What You Need to Know About It
- Raynaud’s Syndrome: Symptoms, Causes, and Treatments
- Learn About These Critical Factors Before Choosing a Medical Equipment Supplier
- Important Considerations for Buying Laboratory Equipment
- Pulse Wave Velocity: A New Feature of Viasonix Falcon
- Peripheral Arterial Disease Diagnostic and Screening Practice Guidelines
- Why is PAD Testing Important to Your Clinic?
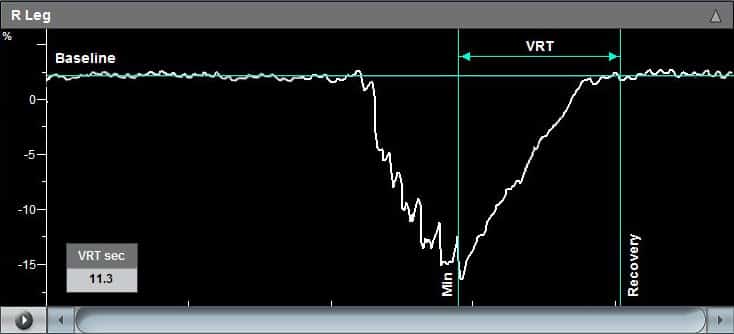
- Venous Reflux
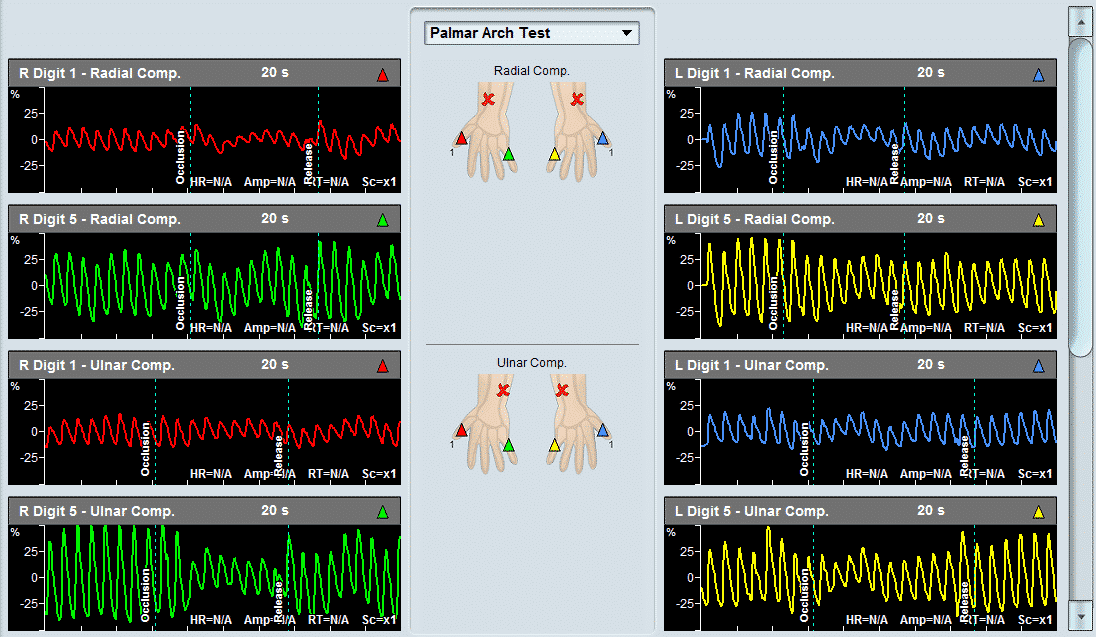
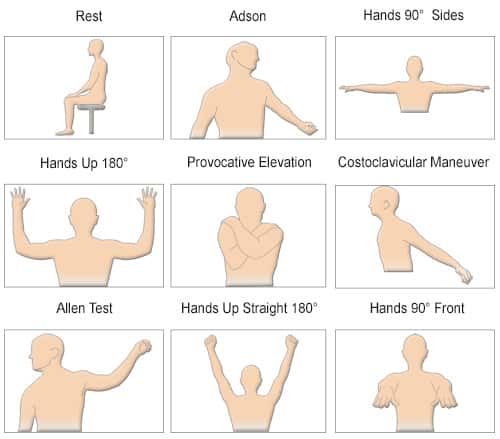
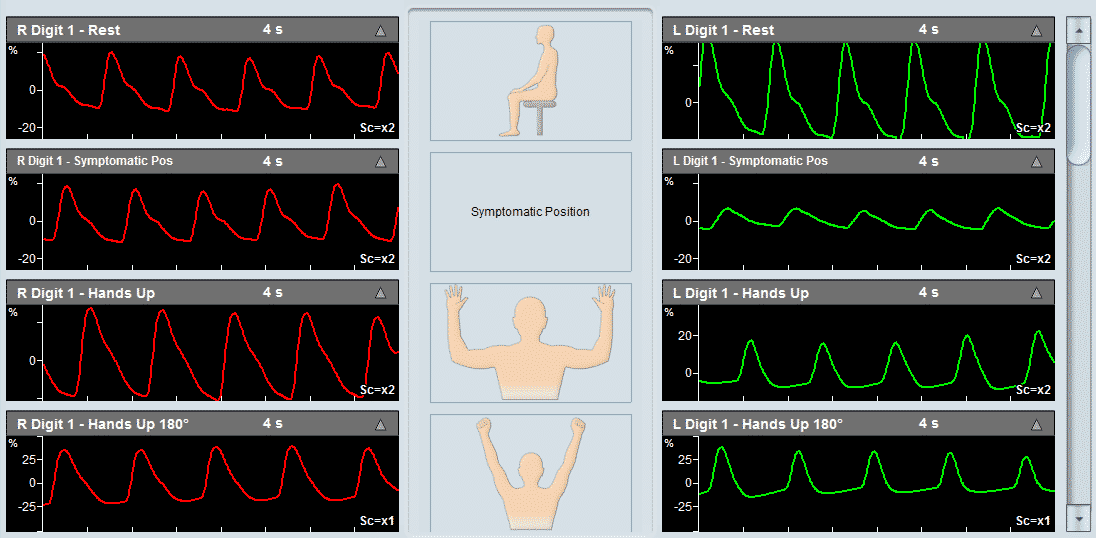
- Thoracic Outlet Syndrome and Palmar Arch Test
- Complete Examination
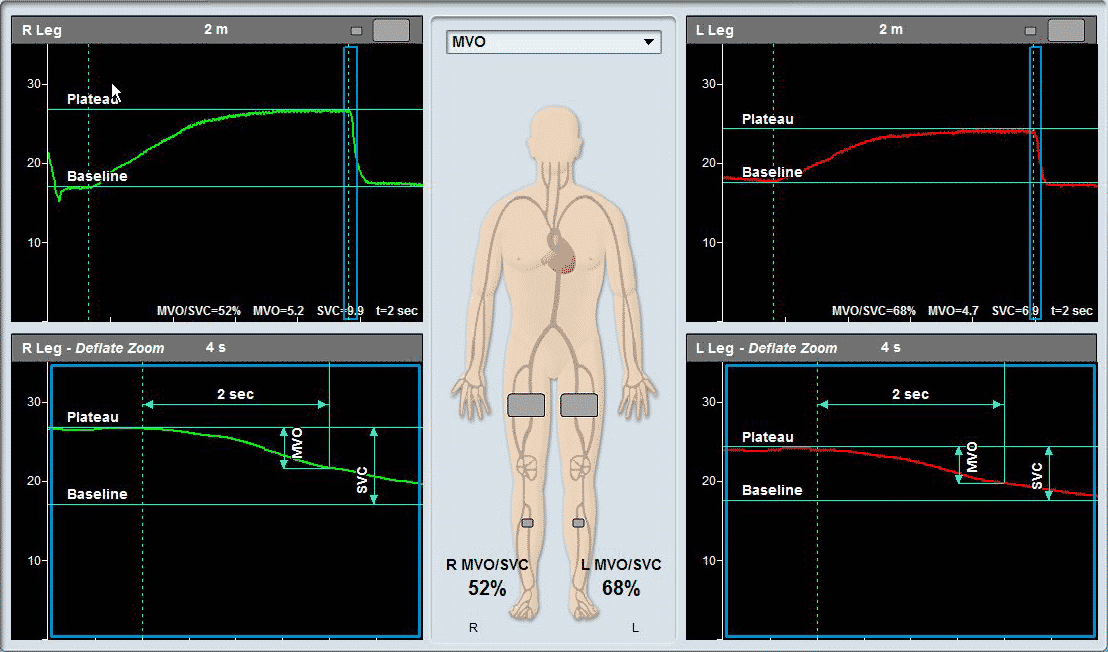
- The Segmental Venous Capacitance / Maximum Venous Outflow (MVO/SVC) Test
Pages
- ABI Machines
- Vascular Doppler Ultrasound
- Peripheral Arterial Disease Testing
- Sitemap
- Falcon Demo
- Contact
- Blog
- Transcranial Doppler
- Vascular Diagnostic Systems
- Falcon Pro
- Venous Reflux
- Toe Brachial Index (TBI)
- Thoracic Outlet Syndrome
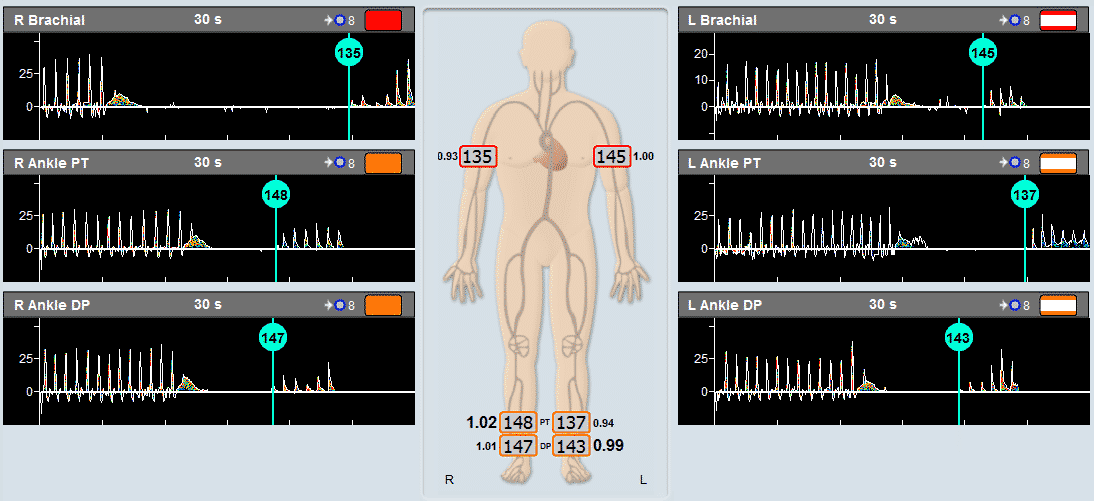
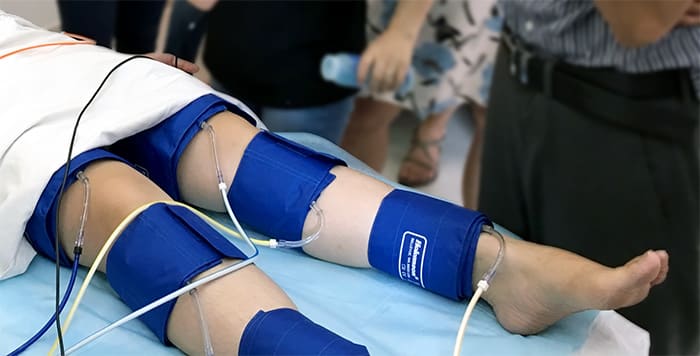
- Segmental Blood Pressures
- Reactive Hyperemia
- Raynaud’s Syndrome
- Pulse Wave Velocity
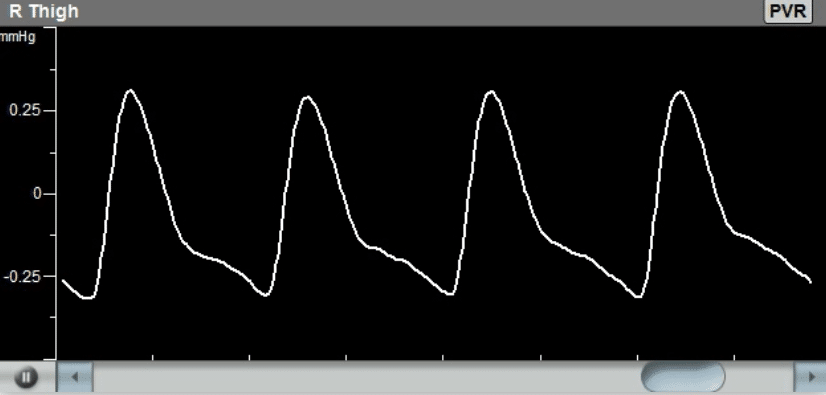
- Pulse Volume Recording
- Photo-Plethysmography Readings
- Penile Function
- Palmar Arch Test and AV Fistula
- Maximum Venous Outflow / Segmental Venous Capacitance (MVO/SVC)
- Extracranial Examination
- Exercise Stress Test
- Doppler Measurements
- Ankle Brachial Index (ABI)
- Air Plethysmography
- About Us
- Home